Managing Type 2 Diabetes Medications — A Pharmacist's Guide
From metformin to Ozempic — a practical guide to the most common Type 2 diabetes medications, how they work, what to watch for, and how your Nepean pharmacist can support your diabetes care.

Understanding Type 2 Diabetes Medications
Type 2 diabetes is the most common form of diabetes, affecting approximately 3.7 million Canadians. Unlike Type 1 diabetes, which is an autoimmune condition requiring insulin from the start, Type 2 diabetes is characterized by insulin resistance — the body produces insulin but does not use it effectively — often combined with a gradual decline in the pancreas's ability to produce enough insulin over time.
The good news is that an impressive range of medications is now available to manage Type 2 diabetes, and many work through very different mechanisms. Understanding how your medications work helps you stay motivated to take them consistently, recognize potential side effects, and have more informed conversations with your healthcare team. This guide covers the main classes of Type 2 diabetes medications available to Ottawa patients, along with practical advice on adherence, monitoring, and what your pharmacist can do to support you.
Metformin — The First-Line Standard
Metformin remains the first medication prescribed for most people with Type 2 diabetes, and for good reason. It has been used for over 60 years, has an excellent safety profile, is inexpensive, and is covered by the Ontario Drug Benefit (ODB) program. Metformin works primarily by reducing the amount of glucose your liver releases into the bloodstream overnight and between meals, and by improving the body's sensitivity to insulin.
Key points about metformin:
- Usually started at a low dose and gradually increased to reduce stomach upset (nausea, diarrhea)
- Should be taken with food to minimize gastrointestinal side effects
- Does not cause low blood sugar (hypoglycemia) on its own
- Lowers A1C by approximately 1–2%
- Must be held temporarily before and after procedures involving contrast dye (e.g., CT scans)
- Should be used cautiously if kidney function is reduced — your pharmacist or doctor will monitor this
SGLT2 Inhibitors — Heart and Kidney Protection
SGLT2 inhibitors — including empagliflozin (Jardiance), dapagliflozin (Farxiga), and canagliflozin (Invokana) — work by blocking the kidneys from reabsorbing glucose, causing excess blood sugar to be excreted in the urine. Beyond their glucose-lowering effect, these medications have demonstrated remarkable cardiovascular and kidney-protective benefits in clinical trials, making them a preferred add-on or even first-choice option for patients with established heart disease, heart failure, or chronic kidney disease.
Important considerations with SGLT2 inhibitors include:
- Increased risk of urinary tract and genital yeast infections — good hygiene is important
- Can cause modest weight loss (2–3 kg on average) and blood pressure reduction
- Risk of a rare but serious condition called DKA (diabetic ketoacidosis) — hold the medication if you are sick, fasting, or having surgery
- Should not be used if kidney function is significantly reduced
- Some brands are now available in generic form, reducing out-of-pocket costs
GLP-1 Agonists — Ozempic, Victoza, and Trulicity
GLP-1 receptor agonists have become one of the most talked-about classes of medications in recent years. Drugs like semaglutide (Ozempic, Rybelsus), liraglutide (Victoza), and dulaglutide (Trulicity) mimic the body's natural incretin hormone GLP-1, which stimulates insulin release in response to meals, suppresses glucagon (which raises blood sugar), slows stomach emptying, and reduces appetite.
The weight loss associated with GLP-1 agonists — particularly Ozempic and its higher-dose counterpart Wegovy — has generated enormous media attention. While these medications can produce clinically significant weight reduction (10–15% of body weight in some patients), their primary role in diabetes management is blood sugar control, and they also carry proven cardiovascular benefits for patients with established heart disease.
Sulfonylureas — Older but Still Useful
Sulfonylureas (glyburide, gliclazide/Diamicron, glimepiride) stimulate the pancreas to produce more insulin. They are inexpensive and effective at lowering blood sugar, but carry a risk of hypoglycemia (low blood sugar) because they work regardless of meal timing. They can also contribute to modest weight gain. Gliclazide (Diamicron MR) is often preferred over older agents like glyburide in older patients because it carries a lower hypoglycemia risk. These medications are fully covered by ODB for eligible Ontario patients.
Hypoglycemia — Recognizing and Managing Low Blood Sugar
Not all diabetes medications cause low blood sugar, but those that do — particularly insulin and sulfonylureas — require patients to know the warning signs and how to respond. Symptoms of hypoglycemia include:
- Shakiness, trembling, or feeling weak
- Sweating, especially cold sweats
- Rapid heartbeat or palpitations
- Dizziness, lightheadedness, or confusion
- Hunger — particularly a sudden, intense craving for sugar
- Pale skin, difficulty concentrating, or irritability
The standard treatment for mild to moderate hypoglycemia is the "Rule of 15": take 15 grams of fast-acting carbohydrate (such as 4 glucose tablets, 150 mL of juice, or 3 teaspoons of sugar dissolved in water), wait 15 minutes, and recheck your blood sugar. If it is still below 4.0 mmol/L, repeat. Carry glucose tablets with you at all times if you take insulin or a sulfonylurea.
Sick Day Rules for Diabetes Patients
Illness, vomiting, and poor appetite change how your body handles blood sugar and how your medications behave. "Sick day rules" are a set of guidelines from Diabetes Canada to help patients navigate these situations safely. In general, when you are sick:
- Continue most diabetes medications even if you are not eating — but check with your pharmacist or doctor about metformin and SGLT2 inhibitors specifically
- Monitor your blood sugar more frequently (every 2–4 hours if possible)
- Stay hydrated — dehydration worsens blood sugar control
- Seek medical attention if blood sugar remains consistently above 15 mmol/L, if you cannot keep fluids down, or if you feel very unwell
- Keep a sick day plan from your diabetes team on hand — ask your pharmacist at Longfields to help you create one
A1C Targets and Annual Monitoring
The A1C test measures your average blood sugar over approximately three months. Diabetes Canada recommends a target A1C of 7.0% or less for most adults with Type 2 diabetes. For frail elderly patients or those with frequent hypoglycemia, a target of up to 8.5% may be more appropriate. Your pharmacist can explain what your A1C result means and how your medications are contributing to your control.
Annual monitoring for people with diabetes should include:
- A1C test every 3–6 months until stable, then every 6 months
- Annual dilated eye exam to check for diabetic retinopathy
- Annual foot examination — including nerve sensation testing
- Annual kidney function tests (eGFR and urine albumin-to-creatinine ratio)
- Annual fasting lipid panel (cholesterol levels)
- Blood pressure monitoring at each visit
- Dental check-up at least annually (diabetes increases gum disease risk)
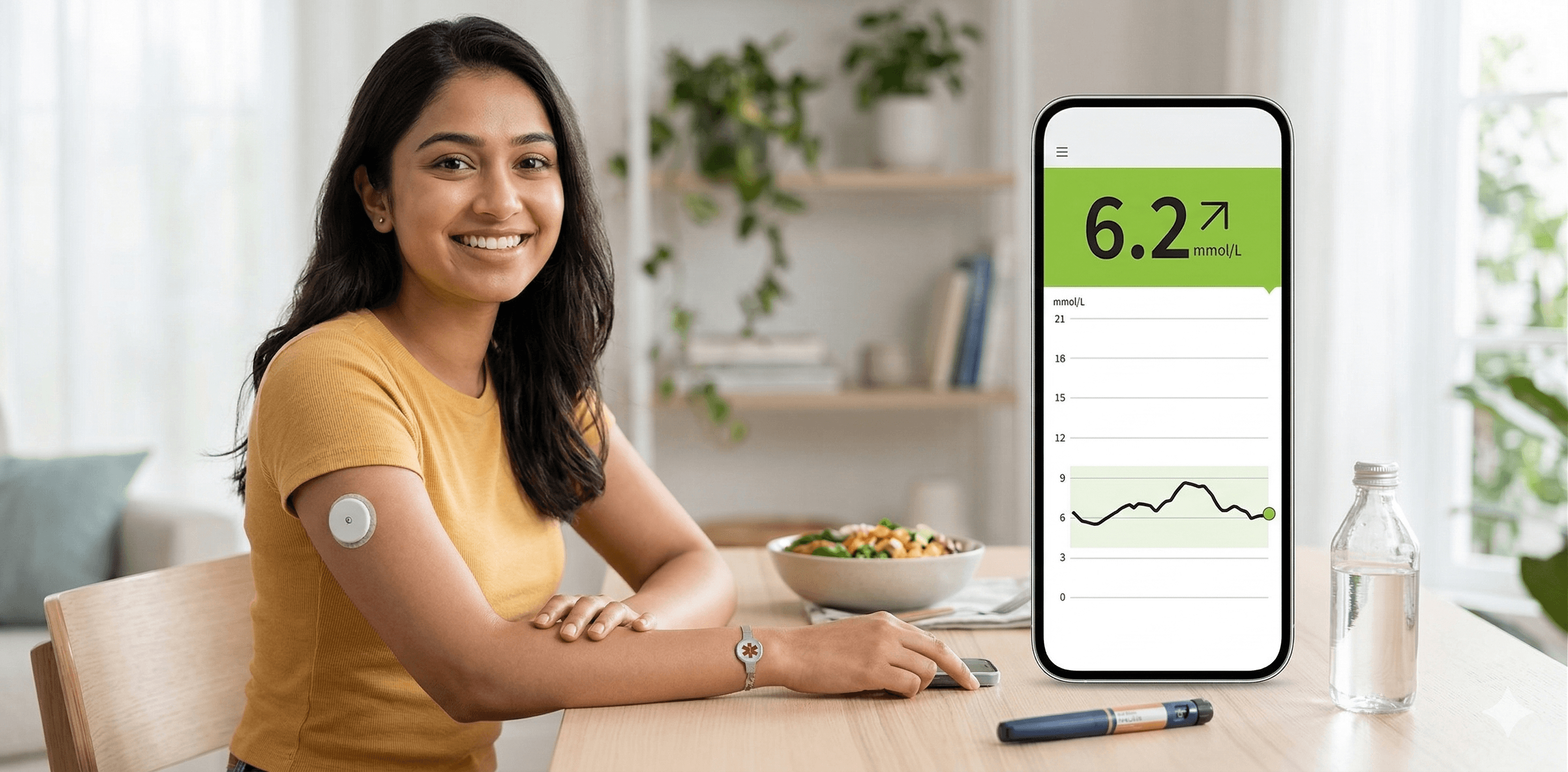
CGM Devices at Longfields Pharmacy
Continuous glucose monitoring (CGM) devices — such as the FreeStyle Libre — have transformed how many people manage diabetes. Instead of pricking your finger multiple times a day, a CGM sensor worn on the arm continuously reads your interstitial glucose and displays the result on a reader or smartphone app. You can also see trends — whether your blood sugar is rising, falling, or stable — which helps you understand how food, activity, and medications affect your levels.
Longfields Pharmacy carries CGM devices and supplies. Ontario's Assistive Devices Program (ADP) and ODB cover FreeStyle Libre sensors for eligible patients with Type 1 diabetes and select Type 2 patients who meet specific criteria. Ask our pharmacists about your eligibility and how to get started with continuous glucose monitoring.
MedsCheck for Diabetes — A Free Pharmacist Consultation
All Ontarians with Type 2 diabetes who take at least one diabetes medication are eligible for a free MedsCheck for Diabetes consultation with their pharmacist. This is a structured, in-depth review of all your medications — not just your diabetes drugs — that covers how each medication works, potential interactions, side effects to watch for, and how your medications relate to your lab results and health goals.
At Longfields Pharmacy, our MedsCheck for Diabetes reviews are thorough and patient-centred. We take the time to answer your questions, explain your A1C results, review your blood sugar log, discuss your monitoring schedule, and coordinate with your family doctor if changes are needed. The consultation is free under OHIP — there is no cost to you. Call us to book your review today.
Related Articles
Medical Disclaimer: The information in this article is intended for general informational purposes only and does not constitute medical advice. Always consult your pharmacist or physician before making any changes to your medications, treatments, or health routine.